Seeing a yellowish tint on your newborn’s perfect skin can send a wave of panic through any new parent. You’re not overreacting. That instinct to scrutinize every detail is your love in action. This guide is designed to be your calm, visual reference in those anxious moments—transforming uncertainty into informed awareness.
This is not a substitute for medical advice. It is a toolkit to help you observe, understand, and communicate effectively with your pediatrician. We’ll walk through what jaundice looks like day-by-day, show you exactly how to check at home, and give you a clear list of signs that mean it’s time to call the doctor.
What Exactly Is Newborn Jaundice? The Simple Science
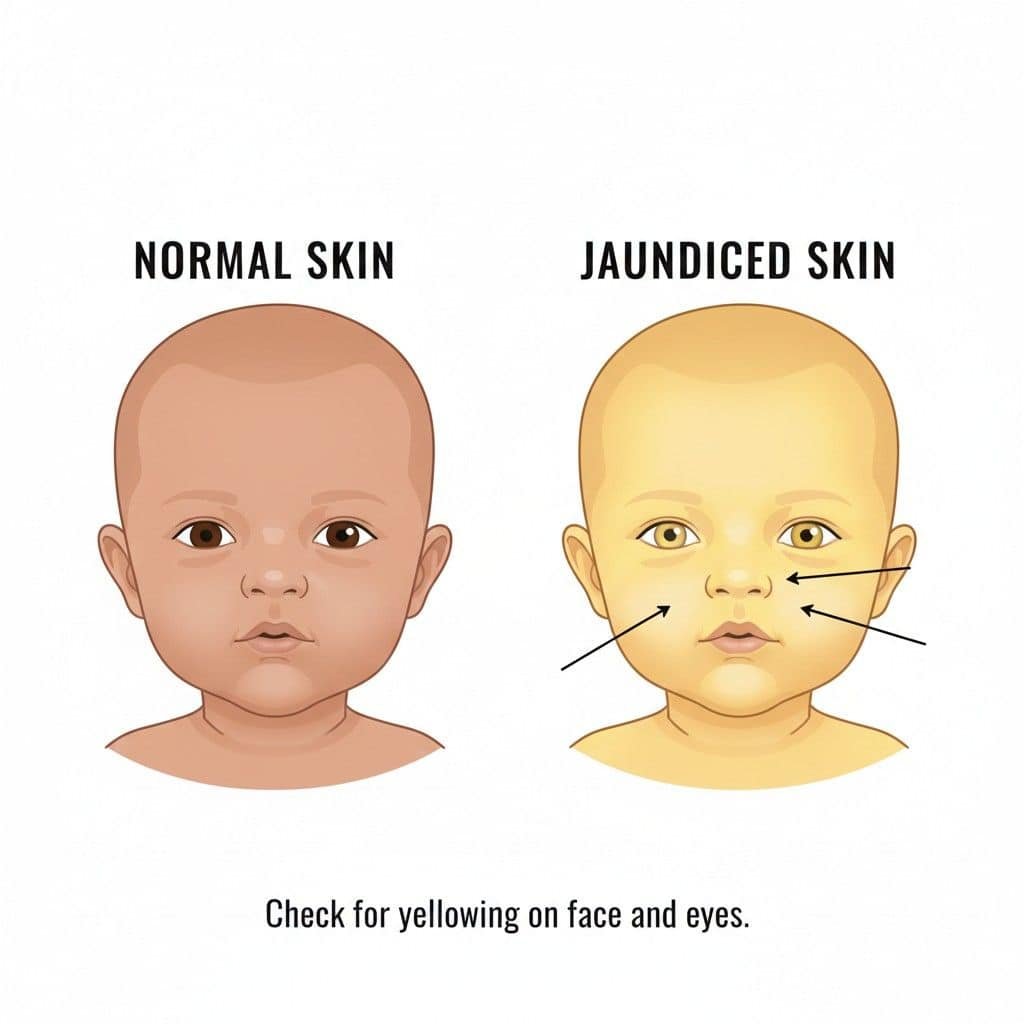
Newborn jaundice is the yellow discoloration of a baby’s skin and eyes. It’s incredibly common, affecting about 3 in 5 full-term babies. It’s not a disease, but a sign that a natural substance called bilirubin has built up in the bloodstream.
Think of it like this: All babies are born with extra red blood cells. As these cells break down naturally, they release bilirubin—a yellow pigment. A newborn’s liver, which is still maturing, is sometimes slower to process and remove this bilirubin. When it builds up, it deposits in the skin and eyes, causing the classic yellow hue.
The Two Main Types: “Wait-and-See” vs. “Call-the-Doctor”
Understanding which type you might be dealing with is key to managing your worry.
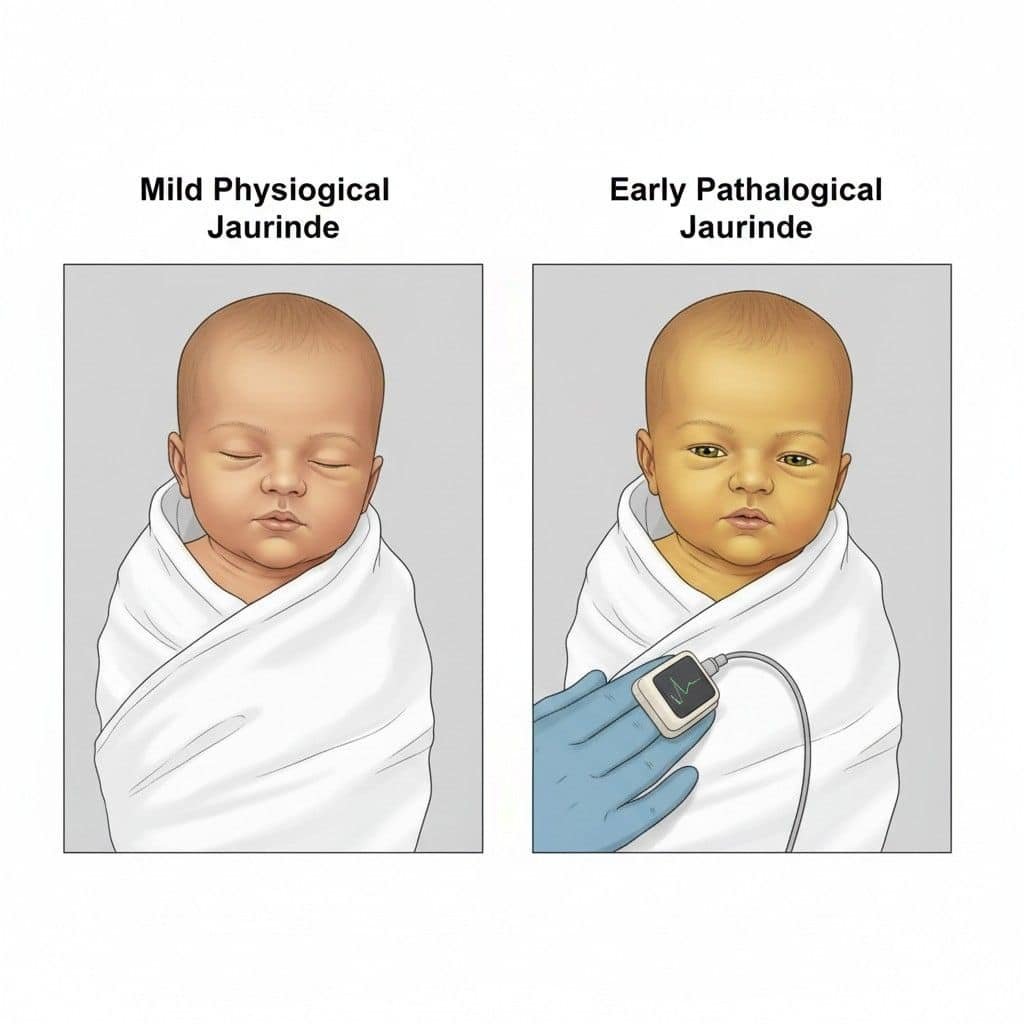
Physiological Jaundice (“Normal”):
Timing: Appears on day 2 or 3, peaks around days 4-5, and usually fades by 2 weeks.
Cause: Simply a newborn liver getting up to speed.
The Baby’s State: Your baby is feeding well, having plenty of wet/dirty diapers, and is alert when awake.
Pathological Jaundice (“Needs Medical Attention”):
Timing: Appears in the first 24 hours of life.
Cause: An underlying issue like blood type incompatibility.
The Action: This requires immediate pediatric evaluation.
A Special Case: Breastfeeding Jaundice This common type is linked to feeding:

Breastfeeding Jaundice: Happens in the first week if baby isn’t getting enough milk. Solution: More frequent, effective feeds.
Breast Milk Jaundice: Appears after week 1, can last a month+, but the baby is perfectly healthy and thriving. Often just needs monitoring.
Your At-Home Toolkit: The Safe “Press Test” & Progression Guide
Before you search frantically for “baby jaundice pictures,” you can perform a simple, safe check. This helps you move from a general worry to a specific observation.
Step 1: The Gold Standard “Press Test”
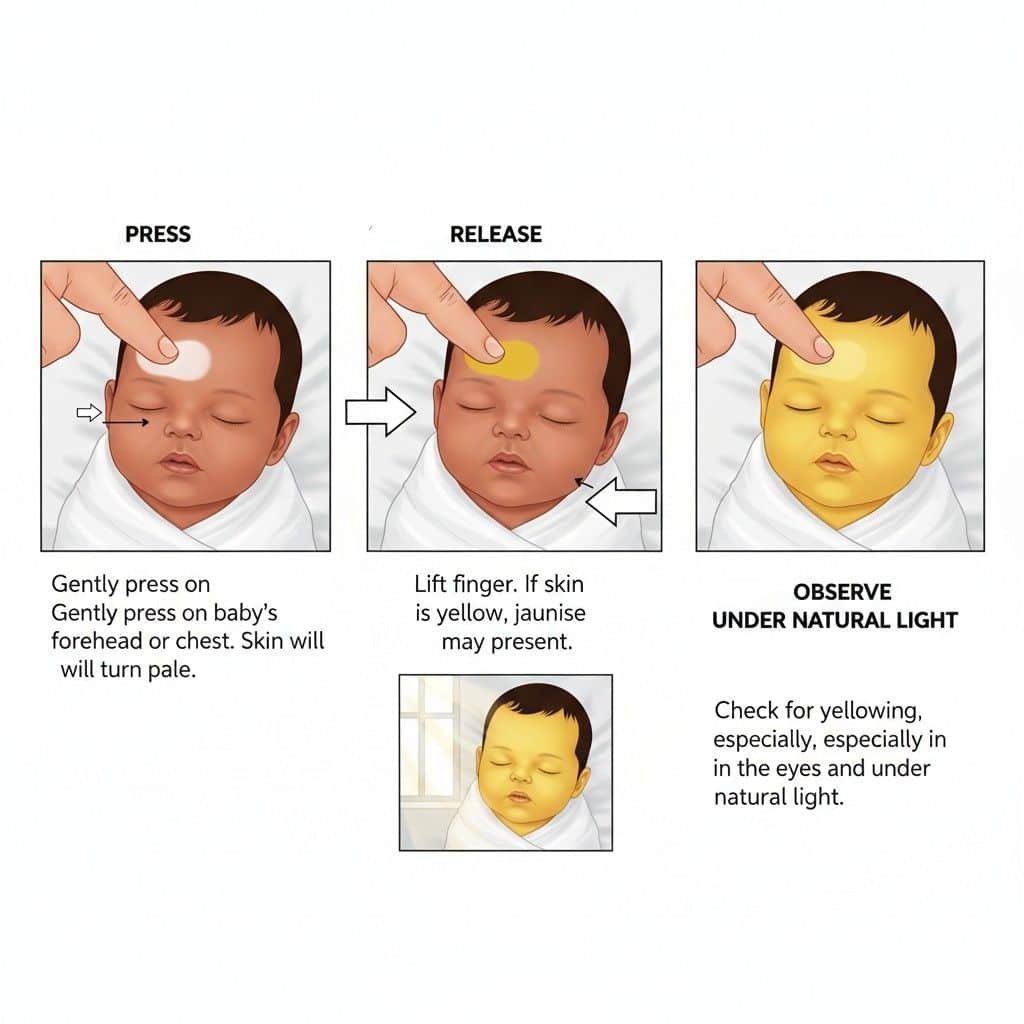
This technique, often called the blanching test, helps you see the true skin tone beneath surface capillaries.
Find Natural Light: Go to a bright window. Artificial light, especially warm-toned lamps, can hide or exaggerate yellowness.
Press Gently: Use a finger to gently press on a bony spot like your baby’s forehead, nose, chest, or shin.
Observe the Release: Quickly release. Watch the color that floods back in that first second.
Normal: Skin looks briefly pale, then returns to its base pink or tone.
Jaundiced: The area shows a distinct yellow tint as blood returns.
Step 2: Understand the “Top-to-Toe” Progression
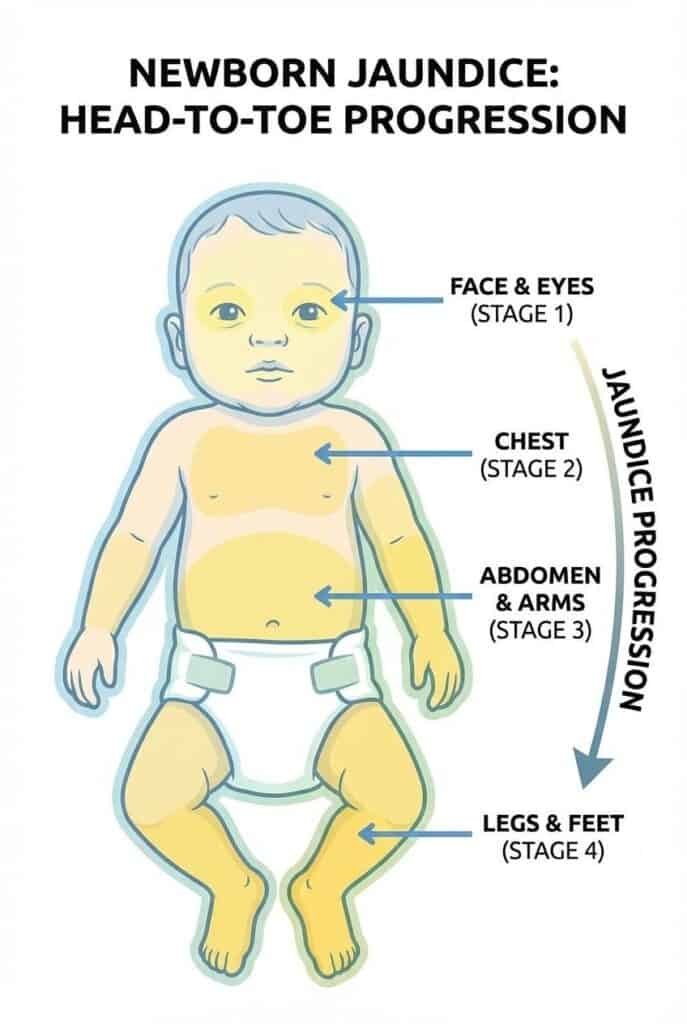
Jaundice typically spreads downward as bilirubin levels rise. Knowing where it is gives you a rough gauge:
Face & Eyes (~5 mg/dL): Common starting point.
Chest & Belly (~10-15 mg/dL): Moderate levels.
Arms & Legs (~15+ mg/dL): Needs pediatric check.
Palms & Soles (>15 mg/dL): A visual sign to call your doctor promptly.
Example: If yellow is only on the face and eyes, it’s likely mild. If it has reached the belly or beyond, it’s time for a professional assessment.
Visual Jaundice Progression: A Day-by-Day Photo Guide (Days 1-10)
This is the visual reference you’ve been looking for. Remember, every baby is unique. Use this gallery as a general guide, not a diagnosis. Your pediatrician’s assessment is what matters most.
Critical Disclaimer: The following descriptions are based on typical patterns. Actual medical evaluation is essential. Jaundice appearing on DAY 1 is always a medical emergency.
(Imagine a clear, slider-based photo gallery here with the following daily descriptions. Each image would have detailed alt-text like “newborn jaundice day 4 example showing yellowing on chest.”)
Days 1-2: The Very Beginning
What You Might See: Often, no visible yellow. The baby’s natural skin tone is most apparent. Key Fact: Any discernible yellow on the face or eyes in the first 24 hours requires an immediate call to your doctor or nurse.
Days 2-4: Common Onset
What You Might See: A subtle, “sun-kissed” or golden hue, often starting on the bridge of the nose and forehead. It may be easiest to see in natural light. The whites of the eyes may begin to look slightly tinged.
Days 4-5: The Typical Peak
What You Might See: The yellow often becomes more obvious and may spread to the upper chest and abdomen. The baby’s eyes may look more clearly yellow. This is when physiological jaundice usually peaks.
Days 6-10: The Fading Phase (With Good Feeding)
What You Might See: With frequent feeding, the yellow begins to retreat from the limbs and belly upward. The face and eyes are often the last to clear. You should see steady daily improvement in color.
The Red Flag Checklist: When to Stop Googling and Start Calling
Trust your instincts. If something feels off, it’s worth a call. Use this checklist. A single “YES” is reason to contact your pediatrician or nurse line immediately.
Visual & Timing Red Flags
- First 24 Hours: Yellow tint appears on day one.
- Rapid Spread: Color moves quickly down the body.
- Deep Discoloration: Baby looks deeply yellow, orange, or even greenish.
- Below the Knees: Yellowing has reached the palms of the hands or soles of the feet.
- Eye Whites: The sclera (whites of the eyes) are brightly yellow.
Behavioral & Feeding Red Flags
- Extreme Lethargy: Baby is very hard to wake, sleeps through feeds, or feels “floppy.”
- Feeding Trouble: Refuses feeds, takes less than 6-8 good feeds in 24 hours.
- Fussiness: Inconsolable crying or an unusual high-pitched cry.
- Poor Output: Fewer than 5-6 wet diapers and 3-4 stools per day by day 5.
- Fever: Rectal temperature of 100.4°F (38°C) or higher.
Why This Matters: While severe complications like kernicterus are rare today, they are why vigilant monitoring exists. Timely treatment is simple and 100% effective at preventing problems.
What the Doctor Will Do: Diagnosis and Treatment Explained
If your pediatrician is concerned, here’s what happens next:
1. Accurate Measurement:
Transcutaneous Meter (TcB): A painless device pressed on the skin that gives a quick estimate.
Serum Bilirubin Test (TSB – the Gold Standard): A tiny heel-prick blood sample gives the exact level in mg/dL.
The magic number isn’t judged alone. Your doctor plots it on an “hour-specific nomogram”—a graph that shows if the level is safe for your baby’s exact age in hours, weight, and gestational age. Context is everything.
2. Effective Treatment Options:
Enhanced Nutrition: For mild cases, frequent feeding (8-12+ times/24hrs) is the primary treatment. It helps baby pass bilirubin in stool.
Phototherapy (“Bili Lights”): The standard, highly effective treatment. Special blue lights help break down bilirubin in the skin so it can be excreted easily.
Hospital Lights: Baby is under overhead lamps.
Home Phototherapy (Bili Blanket): A flexible light pad allows treatment while you hold and feed your baby, promoting bonding.

Myth Bust: Sunlight through a window is NOT a safe or reliable treatment. It risks sunburn, dehydration, and temperature instability while providing inconsistent, weak therapy.
Your Action Plan: Managing Jaundice and Your Anxiety
Feed, Feed, Feed: Wake a sleepy baby to feed every 2-3 hours. Good milk intake is the best natural way to lower bilirubin.
Track Objectively: Use a simple log or our [Free Newborn Wellness Tracker] to note feeds, wet/dirty diapers, and your observations. Data is powerful when talking to your doctor.
Do One Daily Check: Perform the “press test” once a day in consistent natural light. Don’t obsessively check—it fuels anxiety.
Call for Reassurance: Your pediatrician’s nurse line exists for your “Is this normal?” questions. Use it.
Care for Yourself: This stress is real. If anxiety is overwhelming, talk to your partner, a friend, or your doctor. You can’t pour from an empty cup.
Frequently Asked Questions (FAQs)
Q: How long does newborn jaundice last? A: Typical “normal” jaundice peaks around day 5 and clears within 1-2 weeks. Breast milk jaundice can cause a mild tint for 3-12 weeks but is not harmful if the baby is gaining weight well.
Q: Does jaundice mean my baby’s liver is damaged? A: Almost always, no. In physiological and breastfeeding jaundice, the liver is perfectly healthy—it’s just maturing at its own pace. Pathological jaundice requires investigation, but many causes (like blood type differences) are treatable.
Q: Should I stop breastfeeding if my baby has jaundice? A: NO. Stopping can worsen jaundice and disrupt your milk supply. The solution is usually more effective, frequent breastfeeding. Work with a lactation consultant to ensure a good latch and transfer.
Q: My baby has darker skin. How do I check? A: Focus on the whites of the eyes, gums, and palms/soles. The “press test” is especially helpful. Look for a yellow undertone rather than a surface color change.
Q: Are some babies at higher risk? A: Yes. Risk factors include prematurity, bruising from delivery, sibling with jaundice, different blood type from mom, and East Asian ethnicity.
Conclusion: From Worry to Empowered Care

That yellow tint is a visible signal, and as a parent, you are the first to notice. Your vigilance is a strength. This guide aimed to equip that strength with knowledge—showing you how to see clearly, track objectively, and act wisely.
You are not just worrying; you are caring with precision.
Use these tools to partner with your pediatrician. Bring your observations, your logs, and your questions. And always, always honor that inner voice that says, “I should call.” Making that call is the most responsible and loving action you can take.
The journey with newborn jaundice is almost always a temporary one. With informed awareness and a trusted medical team, you will navigate it, and soon this will be just one of the many stories from your baby’s first remarkable days.